|
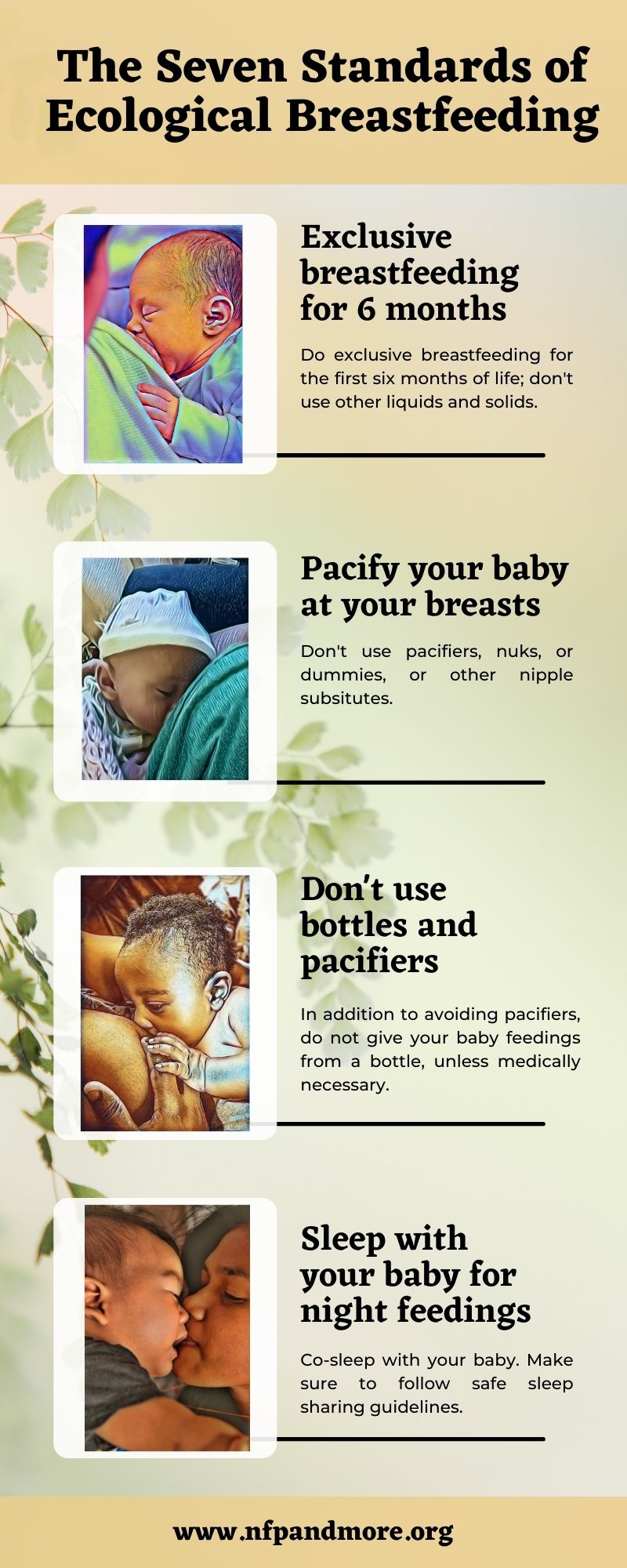
One of my most popular posts in this blog is about ecological breastfeeding. Earlier this year, I was asked by Natural Family Planning International to produce a short video about ecological breastfeeding. I wrote the video, filmed it, acted in it, and edited it. This was a fun experience and I hope to produce more parenting videos in the future! Contact me or comment below if you have ideas for parenting videos, or questions I can answer with a video! Because they go by kind of fast, here are the Seven Standards of Ecological Breastfeeding: Do you have comments or questions about ecological breastfeeding (sometimes called eco-breastfeeding)? Do you have eco-bfing experiences to share? Comment below!
1 Comment
Once a month, Gina Peterson, IBCLC, and Lexy Backstrom, BfNA (two Catholic Nursing Mothers' League leaders) work with me to support Catholic breastfeeding mothers in two online breastfeeding support groups. We launched these groups in March of 2021, and just celebrated our first anniversary of providing free online breastfeeding education and support. This month's topic is "Working with Your Baby's Natural Instincts to Breastfeed." In preparing for our meeting, I took some time to refresh and expand my knowledge of the many instinctual reflexes newborns have at birth that help them to locate, attach, and breastfeed successfully -- when new mothers are given the freedom to hold their healthy, full-term babies skin-to-skin in laid-back, tummy to tummy positions. My interest was piqued by a 2015 research study, "Intrapartum Synthetic Oxytocin Reduce (sic) the Expression of Primitive Reflexes Associated with Breastfeeding." In this study, the researchers observed that those babies exposed to synthetic oxytocin (i.e., "Pitocin") during birth exhibited fewer primitive neonatal reflexes that are favorable to getting started with breastfeeding as compared to the group of babies with no exposure to synthetic oxytocin. The reflexes that appear to be most affected by exposure to Pitocin include all of the rhythmic reflexes that were studied (suck, jaw jerk, and swallowing). As a group, all the primitive neonatal reflexes that were studied were observed less in the group of newborns exposed to synthetic oxytocin as compared to the newborns who were not exposed. The researchers suggested that it may be possible that synthetic oxytocin could cross through both the placenta (which protects the baby from some harmful substances) as well as the barrier that protects the fetus from substances that could damage his or her developing brain. There were several limitations to the study. The group without synthetic oxytocin exposure included more experienced mothers, and the group with exposure had much higher epidural anesthesia rates. However the researchers did not observe any differences in the rates of newborns exhibiting primitive neonatal reflexes based on these two variables. My intention in sharing this information is to encourage healthy mothers to make it a goal to have a natural, unmedicated birth whenever possible -- with a supportive birth team (including a birth doula if possible), in a birthplace that has a track record of good support for natural birth experiences. For healthy moms and babies, a natural birth is the usually the best foundation for breastfeeding. Assuming mother and baby are healthy, mothers can help baby to get started breastfeeding by laying back, supporting her body in a semi-reclined ("laid-back") position and place baby skin-to-skin and tummy to tummy, allowing baby to self-attach. Of course, even if Pitocin is necessary during a particular mother's birth, this does not mean she and her baby will be unable to breastfeed! My first birth was augmented with Pitocin and my fifth birth was induced with Pitocin, yet both of these babies successfully breastfed into early childhood. In any birth requiring the use of medications, (as well as all natural births!) make sure to get some of each of the four components that help you to succeed when you breastfeed:
As I know from my own experiences, breastfeeding is NOT always easy. And despite doing everything "right", it can be frustrating, exhausting, and sometimes just plain hard work that seems impossible. Your breastfeeding journey is unique to you and your baby; and as always, what works for both of you is what's best for you. Contact me if you need a listening ear or another perspective! resources
Chris Hagen gave another donation this month and became a Gold Community Sponsor. SCBP is a nonprofit registered in the state of Minnesota. A very large portion of our income is made of financial gifts from individuals like you! Chris's gift will help us keep our doors open so we can continue to provide free and low-cost birth, breastfeeding, and parenting services to growing families and families of loss throughout the USA. Thanks, Chris!
Chris Hagen became St. Croix Birth & Parenting's newest Crystal Community Sponsor. SCBP is a nonprofit registered in the state of Minnesota. A very large portion of our income is made of financial gifts from individuals like you! Chris's gift will help us keep our doors open so we can continue to provide free and low-cost birth, breastfeeding, and parenting services to growing families and families of loss throughout the USA. Thanks, Chris!
8/12/2021 supporting new MOTHERs during a loCkdown: a guide for friends and extended familyRead NowThe coronavirus pandemic has changed life as most of us once experienced it. Many areas of the world are in lockdown, and even in areas where things have opened up, as the number of COVID-19 cases spikes again, we will likely face more social distancing measures or quarantines to try to slow the spread (if we aren't already). For some new mothers, this slower, more home-based pace of life has been a good thing. These moms report that being quarantined with their babies has helped them breastfeed, since - just to mention one thing - being separated from a nursing baby tends to make maintaining a milk supply more challenging and if nothing else, lockdown gives us lots and lots of time with our immediate family members. But in other and important ways, social isolation is not great for new mothers. Many important services that mothers need, including lactation help, have been more difficult or impossible to access during lockdown. Aside from access to healthcare, all mothers need other mothers, friends, sisters, cousins, grandmothers, aunts...we need our sisters and our sage femmes to let us know we're not alone; we're loved; we're doing a good-enough job; our kids are normal (usually); and, if they're not, to have faith that eventually, this too shall pass. Lockdowns put a lock on these face-to-face and side-by-side moments...natural social interactions which normally serve to lower our stress levels and restore us - "enhope" us. And all this goes quadruple for new mothers. Dealing with lochia, sore nipples, night feeds, blow outs, the constant guessing games that a newborn brings (a/k/a no instruction manual), keeping a brand new non-verbal human thriving and growing, and caring for everything "down there" is just a lot. In some idealized past, we imagine our ancestral mothers got to lie around while their loving, supportive kin waited on them hand and foot. Sure, maybe that happened sometime, somewhere, but envying our long-departed great-great-grandmother's "lying in" is not really going to help you get through this painful feed, on this lonely day, at this ungodly hour. So let's break this down. New mothers have physical needs. Food, water, monster sized maternity pads (in the beginning), menstrual pads later on, baths or showers, and (eventually) clean clothes. If you love her, ask about these things. If she needs something, help or ask someone else to help. Leave things on her porch, in her mailbox, send it unaccompanied up the elevator, or throw it through her window if you have to! (Or you could just give to the baby's dad, but that's not as fun.) If she's good with her physical needs, I guarantee she has emotional needs. Call and ask about her birth. Listen. Bite your tongue if you find yourself starting any sentence with the words "at least." Listen. Celebrate the good stuff with her. Mourn with her anything she found sad. Share her anger if anything made her mad. Don't tell her what she should have done differently. Listen. Are you listening? Keep listening. No matter what, make sure to let her know how amazing she is. No one in the history of the world had her birth. It was her adventure and she is a heroine for having done it! Call another time and ask how things are going with the baby. Celebrate the joys. Mourn the things that aren't going so well with her. Did I mention don't tell her she should have done anything differently? She is probably already beating herself up about something. If her baby is growing and developing, she's doing a great job. Tell her. If her baby is struggling, offer to help. If she's got other kids, depending on your local situation, you might be able to have someone in mom's social bubble bring the baby's older siblings somewhere outside for a socially distanced / masked playdate so she can visit (whether in-person or virtual) with the doctor, or the chiropractor, or the lactation consultant, or whoever it is she thinks can help. Moms grow in confidence and feel capable when the people around them support their decisions about their baby's care. Be that person (even if you secretly disagree). Being a great friend / sister / mother / mother-in-law, etc., means supporting the new mom's efforts to become a mother, a big part of which is taking responsibility for her baby. And chances are very good that if the baby continues to struggle, even after that visit with [insert name here] she will try something else, and something else, and something else, and maybe, when she's tried everything else, she may even ask you for your advice! Now is your moment. A few days or a week later, call her again. And then again. And yet again. And pretty soon she will blossom and her tiny baby will become a chunky monkey, roll over and crawl and take his first steps, and life will settle and she will never forget that you were there, on the sidelines, cheering her on the whole time. Maybe you never carried a meal to her bedside on a solid-gold tray, but you were there. And maybe she'll tell her great-great-granddaughters about you and how you were there for her when great-grandpa was born, during the time of the world coronavirus pandemic. ways st. croix birth & Parenting can help
Quick Baby Rubdown! 3 minute massage for baby. Easy to fit in after a bath or to relax baby before bedtime. Infant Massage has many benefits for your baby, including better mental health into adulthood! This video is a mini version of the full body infant massage in our Infant Massage Basics class! Check our schedule for our next online class. Contact us to register! This video is intended for educational purposes only. Please consult your baby's doctor or medical care provider for specific advice about the care of your baby. It is not recommended that you use any oil on babies under 6 weeks of age. Consult with a certified aromatherapist or your baby's doctor concerning the use of essential oils on babies younger than three months old.
c. Christelle Hagen 2021 ~~~~~~~~~~~~~~~ Music Credits: Birthday Musician: LiQWID URL: http://soundcloud.com/liqwid Did you know holding your baby tummy to tummy and skin to skin counts as tummy time? In Bosom Buddies: Tummy to Tummy, Skin to Skin (BONUS Tummy Time Activity Video) you will learn:
This video is intended for educational purposes only. Please consult your baby's doctor or medical care provider for specific advice about the care of your baby. Music Credits:
Call Me Musician: LiQWID URL: http://soundcloud.com/LiQWID Birthday Musician: LiQWID URL: http://soundcloud.com/liqwid Someday Musician: Alexander Delarge URL: https://icons8.com/music Words Musician: Jason Shaw URL: https://audionautix.com License: https://creativecommons.org/licenses/... Ice cream Musician: Ilya Truhanov URL: https://icons8.com/music Help your baby's tummy time take off with the Airplane Game! No equipment needed. In Up, Up, and Away! (Tummy Time Activity Video #4) you will learn:
This video is intended for educational purposes only. Please consult with your baby's doctor or medical care provider for specific advice about the care of your baby. Music Credits
Folk Bed Musician: Jason Shaw URL: https://audionautix.com License: https://creativecommons.org/licenses/by/4.0/legalcode Lazy Day Musician: Jason Shaw URL: https://audionautix.com Ice Cream Musician: Ilya Truhanov URL: https://icons8.com/music Don't Stop Now Musician: ASHUTOSH URL: https://soundcloud.com/grandakt Rock your baby's tummy time by using a large ball! Rock 'n' Roll Your Baby (Tummy Time Activity Video #3) explains how to:
This video is intended for educational purposes only. Please consult your baby's doctor or medical care provider for specific advice about the care of your baby. Always follow any baby carrier's instructions for safe babywearing and ensure baby's airway is straight so they can breathe freely. Music Credits
Chill Musician: LIQWID URL: http://soundcloud.com/liqwid Ice Cream Musician: Ilya Truhanov URL: https://icons8.co/music Lazy Day Musician: Jason Shaw URL: https://audionautix.com/ Sweet Musician: LIQWID URL: http://soundcloud.com/liqwid Use safe mirror play to make tummy time more enjoyable for your baby! Who's that Baby in the Mirror? (Rumble Tumble Tummy Time Activity Video #2) explains how to:
Music Credits:
Lazy Day Musician: Jason Shaw URL: https://audionautix.com Tiny People Musician: Alexei De Bronhe URL: https://icons8.com/music Ice Cream Musician: Ilya Truhanov URL: https://icons8.com/music Whenever Musician: LiQWYD URL: http://www.soundcloud.com/liqwyd |
Details
Archives
November 2023
Categories
All
Enter Your Email Address to get St. Croix Birth Blog Posts in Your Inbox(We don't collect your email address and you won't get anything else from us.)
|






 RSS Feed
RSS Feed